A
Active disease: Disease state characterized by active, ongoing inflammation due to vasculitis. In this state, vasculitis causes damage to organs. Treatment is initiated to induce disease remission.
Alkylating agents: A group of drugs originally used to treat cancer, now used (in lower doses) to treat some forms of severe vasculitis.
ANCA: Anti-neutrophil cytoplasmic antibodies. The abbreviation is pronounced just like the last name of the singer, Paul Anka. These antibodies are found in patients with some forms of vasculitis, particularly granulomatosis with polyangiitis, microscopic polyangiitis, and the Churg-Strauss syndrome.
Anemia: A low hematocrit (roughly corresponding to a low red blood cell count).
Anesthesic: Means literally “without feeling”. A drug administered for medical or surgical purposes, that induces partial or total loss of sensation. An anesthesic may be topical, local, regional, or general, depending on the method of administration and area of the body affected.
Aneurysms: Weakening of a blood vessel wall by inflammation. Sometimes leads to rupture of the vessel.
Angiogram: An X-ray representation of blood vessels made after the injection of a radio-opaque dye. Used to visualize the inner layer of blood vessels and to determine the location and degree of narrowing or dilation.
Antibodies: A Y-shaped protein on the surface of B cells that is secreted into the blood in response to a challenge to the immune system, such as a bacterium, virus, parasite, or transplanted organ. Antibodies neutralize foreign proteins by binding specifically to them. Antibodies are also known as immunoglobulins.
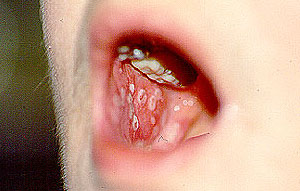
Aphthous ulcers: Ulcerations on the mucous membranes of the mouth or genitals, often caused by an infection or trauma. Aphthous ulcers also occur in Behcet’s disease and connective tissue diseases such as Lupus.
Arthralgias: Aches or pains in joints, without obvious swelling, warmth, or redness.
Arthritis: Inflammation of a joint, usually accompanied by pain, swelling, and stiffness, and resulting from infection, trauma, degenerative changes, metabolic disturbances, or other causes. Arthritis occurs in various forms, such as the arthritis associated with infections, osteoarthritis, or rheumatoid arthritis. Many forms of vasculitis can also be associated with arthritis.
Aseptic: Using sterile techniques or methods to protect against infection by microbes.
Asymmetrical: Having no balance or symmetry. Different on the left side of the body as compared to the right. “Asymmetric weakness of the left lower extremity” means that the left leg is weak but the right is not.
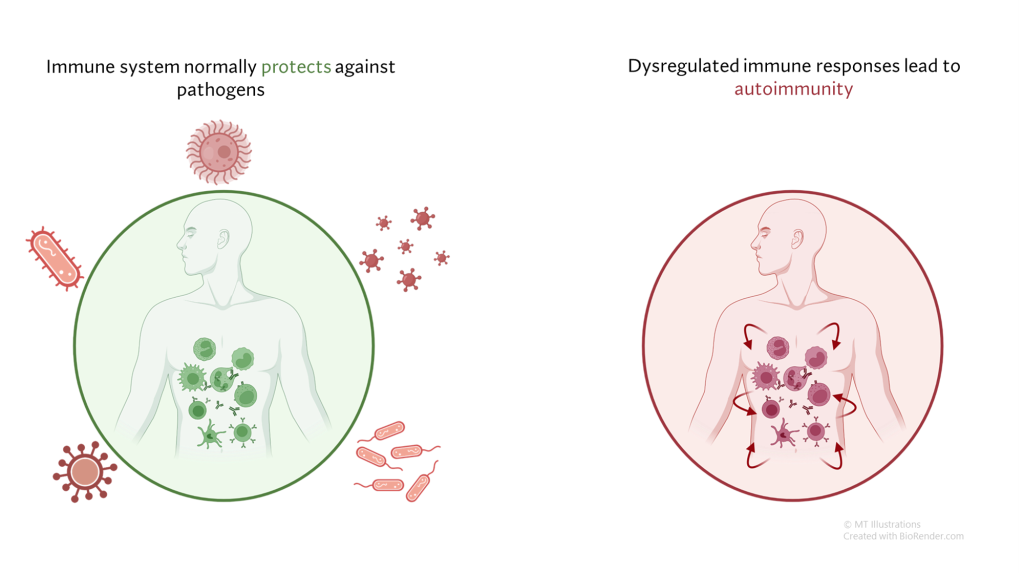
Autoimmune: Relating to an immune response by the body against one of its own tissues; for example, its own cells, molecules, or organs. Autoimmune diseases often involve the formation of antibodies directed against specific body tissues, such as parts of the kidney or blood vessel walls.
B
Beading: The appearance of a blood vessel as of a string of beads, with alternating areas of narrowing and dilation.
Biopsy: Removal of a piece of a tissue or organ through either surgery or sampling with a needle to determine the existence or cause of a disease.
C
Capillaries: The smallest blood vessel in the body. Capillaries connect arterioles (small arteries) with venules (small veins). Capillaries form an intricate network throughout the body for the interchange of various substances, such as oxygen and carbon dioxide, between blood and tissue cells.
Casts: A cluster of cells or proteins formed in the kidney and excreted in the urine. Red blood cell casts usually indicate the presence of active vasculitis within the kidney. Kidney vasculitis is also known as glomerulonephritis.
CAT Scan (CT scan): A Computerized Axial Tomography scan is an x-ray tube that rotates in a circle around the patient, making many pictures as it rotates. The multiple x-ray pictures are reconstructed by a computer in cross-sectional images, permitting doctors to examine “slices” through different organs.
Catheterization: The insertion of a small plastic tube into a blood vessel, for the purpose of infusing fluid or radio-opaque dye (as in angiography), or for the purpose of sampling blood.
Cavity: A hollow area within the body.
Chlorambucil: A medication used to depress lymphocytic production and maturation. The brand name for this medication is Leukeran.
Claudication: A symptom caused by lack of blood flow to the muscles caused by narrowing of the arteries. The symptom of claudication usually occurs in the calf or in an arm, and is an aching pain that resolves with rest.
Conjunctivitis: Inflammation of the most superficial layer of the eye, characterized by redness and often accompanied by a discharge. Conjunctivitis can be caused by certain infections, but is also associated with some types of vasculitis.
Constitutional: Symptoms Symptoms that relate to the entire body as a whole, rather than to an individual organ. Constitutional symptoms include fatigue, malaise, and weight loss.
Crescent: A shape resembling the curved shape of the moon in its first or last quarters. With regard to vasculitis, a crescent is a pathological finding in the kidney that is observed under the microscope. Crescents are caused by damage to glomeruli, the individual blood-filtering units within the kidney.
Cutaneous: Relating to, existing on, or affecting the skin.
Cyclophospamide: An alkylating agent used in combination with corticosteroids (such as prednisone) to treat serve cases of vasculitis.
Cystoscopy: The inspection of the interior of the bladder using a lighted tubular endoscope, inserted through the urethra. The major reason for performing cystoscopy in patients with vasculitis is to screen for bladder injury caused by cyclophosphamide.
Cytoplasmic: The protoplasm outside the nucleus of a cell.
D
Dermis: The layer of the skin located below the epidermis, containing nerve endings, sweat and sebaceous glands, and blood and lymph vessels. Small and medium-vessel forms of vasculitis affect the dermis and sometimes the layer just below the dermis; the subcutaneous fat.
Dialysis: A pathological deficiency in the oxygen-carrying component of the blood, measured in unit volume concentrations of hemoglobin, red blood cell volume, or red blood cell number.
E
Eosinophils: A type of white blood cell containing cytoplasmic granules that are stained easily by eosin or other acid dyes.
Epidermis: The protective outer layer of the skin.
ESR: Erythrocyte Sedimentation Rate is the rate at which red blood cells settle out in a tube of blood under standardized conditions; a high rate usually indicates the presence of inflammation.
Etiology: The cause or origin of a disease.
G
Gangrene: Death and decay of body tissue, often occurring in a limb, caused by insufficient blood supply and usually following injury or disease.
Glomerulonephritis: Inflammation in the kidney, characterized often by decreased production of urine and by the presence of blood and protein in the urine.
Glomerulus: A tuft of capillaries within the kidney that filters blood in order to form urine. Normally, each kidney has approximately 1 million glomeruli.
H
Hematuria: The presence of blood in the urine.
Hyperpigmented: An excess of pigment (color) in a tissue. For example, in some patients, parts of the skin affected by vasculitis become hyperpigmented after the vasculitis has resolved.
I
IgA: Immunoglobulin A. A specific subcategory of antibodies (which all individuals have). For reasons that are not understood, IgA deposits within the blood vessels of the skin, joints, kidney, and GI tract in Henoch-Schonlein purpura, leading to vasculitis.
Incident/incidence: The number of new cases of a disease in a population over a period of time. Physicians often refer to the “annual incidence” of a given disease; that is, the number of new cases occurring each year.
Infarction: Localized necrosis resulting from obstruction of the blood supply. Myocardial infarction is another name for a heart attack.
Infection: Invasion by and multiplication of pathogenic microorganisms in part of the body, or in the body’s bloodstream.
Infiltrates: A collection of inflammatory cells within a body tissue; for example, in the lung. Pulmonary infiltrates are visible on chest x-rays in pneumonia and in some forms of vasculitis.
Inflammation: A localized protective response of the body tissues to injury, irritation, or infection; characterized by pain, swelling, redness, and heat. Vasculitis is inflammation within the blood vessels.
Intravenous: A drug, nutrient solution, or other substance administered into a vein.
Invasive: Relating to a medical procedure in which a part of the body is entered, as by puncture or incision. Invasive procedures such as tissue biopsies or angiograms are sometimes necessary to diagnose vasculitis.
Ischemia: A decrease in the blood supply to an organ, tissue, or body part caused by constriction or obstruction of the blood vessels.
L
Lesion: A wound or injury. A localized pathological change in a bodily organ or tissue. An infected or diseased patch of skin.
Localized: Restricted or limited to a specific body part or region: localized pain and numbness.
Lupus: A systemic disease that results from an autoimmune mechanism. Individuals with lupus produce antibodies to their own body tissues. The resultant inflammation can cause kidney damage, arthritis, pericarditis, and, sometimes, vasculitis.
M
Meninges: The three membranes that cover the brain and spinal cord. The three layers are called the arachnoid (the “spider-like” innermost layer), the pia mater (the middle layer), and the dura mater (the “tough mother” outermost layer).
Mesenteric: Relating to folds of the peritoneum (the abdominal cavity) that connect the intestines to the abdominal wall, especially such a fold that envelops the small intestine.
Mimicker: A disease process that imitates or simulates another. For example, the lung lesions of granulomatosis with polyangiitis may be mimickers of tuberculosis.
MRI Magnetic Resonance Imaging: Another fancy x-ray, similar to a CT scan. MRI scans also provide cross-sectional images of body organs. Because MRI technology involves the use of a large magnet, people with pacemakers, metallic aneurysm clips, and other metallic inserts are not eligible to have these studies.
Myeloperoxidase Abbreviated MPO: An enzyme found in many tissues and cells throughout the body. For reasons that are unknown, many patients with granulomatosis with polyangiitis and microscopic polyangiitis make antibodies to this protein.
N
Nasal septum: A thin wall dividing the nasal cavity into two halves.
Neuropathy: A disease or abnormality of peripheral nerves, the nerves that mediate sensation and movement in the arms, legs, and other body parts.
O
Occlusion: An obstruction or a closure of a blood vessel.
Opportunistic infections: A pathological deficiency in the oxygen-carrying component of the blood, measured in unit volume concentrations of hemoglobin, red blood cell volume, or red blood cell number.
Otitis media: Inflammation of the middle ear (the space just behind the eardrum). This may occur because of an infection or as a result of some forms of vasculitis, such as granulomatosis with polyangiitis.
P
Palpable: Perceptible to touch; capable of being palpated.
Pathologist: A physician who examines tissue biopsies for the purpose of determining the precise cause of disease.
Perforation: A hole in an organ, such as the gastrointestinal tract.
Perinuclear: Of or pertaining to a nucleus; situated around a nucleus. In some forms of vasculitis (e.g., microscopic polyangiitis), anti-neutrophil cytoplasmic antibodies (ANCA) cause perinuclear staining on immunofluorescence tests.
Pneumonia: An acute or chronic disease marked by inflammation of the lungs and caused by viruses, bacteria, or other microorganisms. Forms of vasculitis that involve the lung are often misdiagnosed as pneumonia. Pneumonia is also a type of opportunistic infection that may occur in vasculitis patients under treatment.
Prevalence: The total number of cases of a disease present within a given population at a particular time. The prevalence of giant cell arteritis in the United States, for example is estimated to be 160,000.
Proteinuria: The presence of excessive amounts of protein in the urine. Proteinuria is usually caused by damage to the kidneys.
Purpura: A condition characterized by small amounts of bleeding into the skin and mucous membranes that result in the appearance of purplish spots or patches.
R
Raynaud’s phenomenon: Spasm of the arteries to the fingers and/or toes, resulting in blanching or pain.
Remission: When vasculitis has been treated to the point that there are no signs or symptoms of ongoing active inflammation. In this state, patient may experience symptoms related to damage from prior disease activity, but no active inflammation is present.
Retinal: The innermost layer of the eye. Serves as the eye’s camera, transmitting images to the brain via the optic nerve.
Rheumatologist: A physician who specializes in the diagnosis and treatment of diseases in which the immune system has gone awry, leading to inflammation in a variety of organs.
S
Sclera: The white part of the eye. “Scleritis” is a type of inflammation that occurs in the sclera in some forms of vasculitis.
Stenosis: A constriction or narrowing of a blood vessel.
Steroid-sparing drug: An immunosuppressive drug that has the benefits of prednisone but does not cause as many side effects.
Subcutaneous: Underneath the skin. Some medications, for example, are injected under the skin.
Systemic: Relating to a system or relating to, or affecting the entire body or an entire organism.
T
Teratogenic potential: The risk of causing birth defects. Some medications are said to have “teratogenic potential”.
Thrombosis: A blood clot.
U
Urinalysis: Laboratory analysis of urine, used to aid in the diagnosis of disease or to detect the presence of a specific substance. In vasculitis, the urinalysis is used to detect protein, blood, or clumps of blood cells in the urine. All of these findings may suggest kidney inflammation.
Uveitis: Inflammation within either the anterior (front) or posterior (back) part of the eye.
V
Vasculitis: What this website is all about!